Pulmonary Embolism
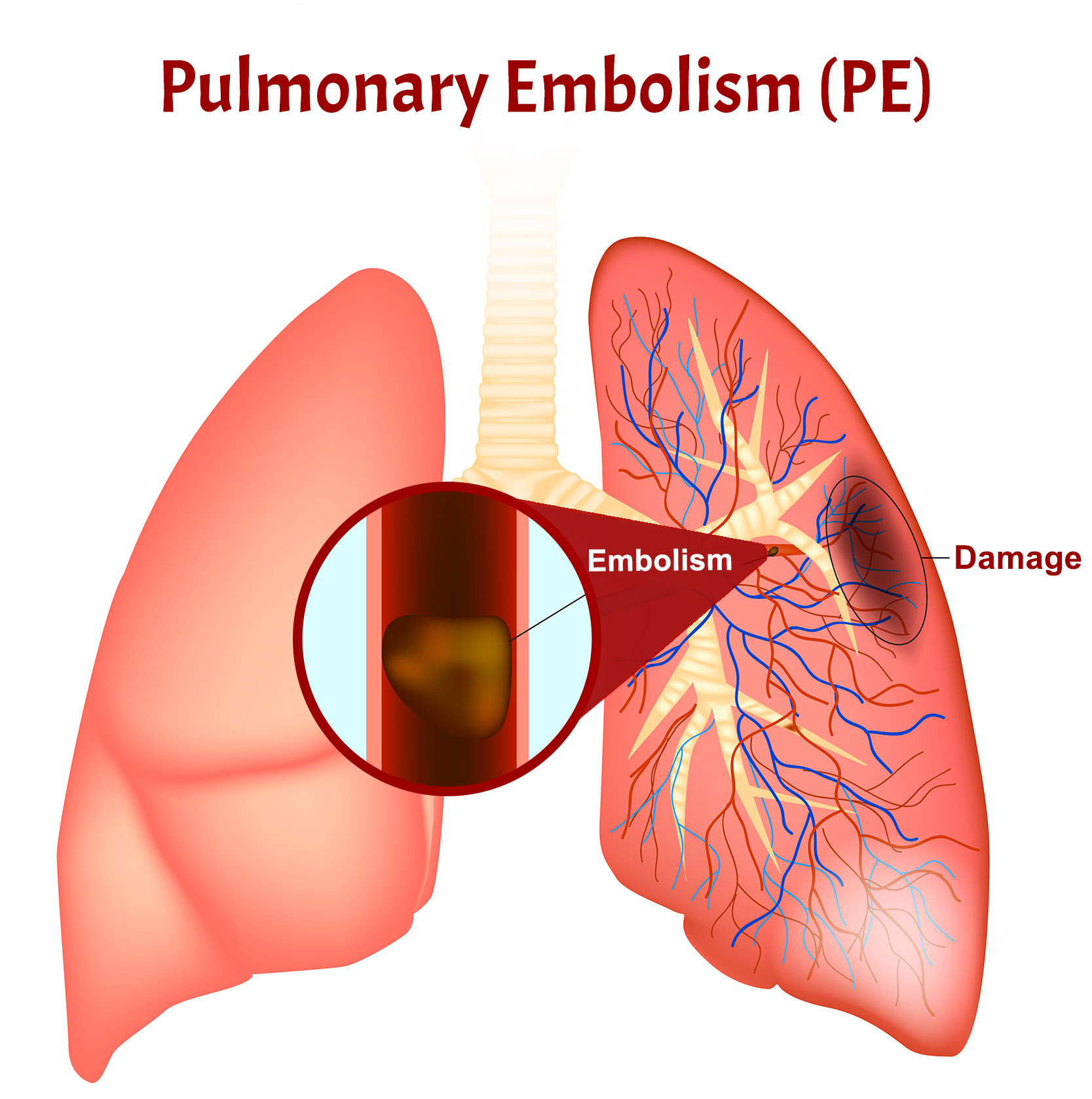
Pulmonary embolism (PULL-mun-ary EM-bo-lizm), or PE, is a sudden blockage in a lung artery. The blockage usually is caused by a blood clot that travels to the lung from a vein in the leg.
A clot that forms in one part of the body and travels in the bloodstream to another part of the body is called an embolus (EM-bo-lus).
PE is a serious condition that can:
- Damage part of your lung because of a lack of blood flow to your lung tissue. This damage may lead to pulmonary hypertension(increased pressure in the pulmonary arteries).
- Cause low oxygen levels in your blood.
- Damage other organs in your body because of a lack of oxygen.
If a blood clot is large, or if there are many clots, PE can cause death.
Other Names for Pulmonary Embolism
- Venous thromboembolism (VTE). This term is used for both pulmonary embolism and deep vein thrombosis.
- Causes
- Risk Factors
- Symptoms
- Screening and Prevention
- Diagnosis
- Treatment
- Living with PE
- Clinical Trials
- Publications
Overview
PE most often is a complication of a condition called deep vein thrombosis (DVT). In DVT, blood clots form in the deep veins of the body—most often in the legs. These clots can break free, travel through the bloodstream to the lungs, and block an artery.
Deep vein clots are not like clots in veins close to the skin’s surface. Those clots remain in place and do not cause PE.
The exact number of people affected by DVT and PE isn’t known. Estimates suggest these conditions affect 300,000 to 600,000 people in the United States each year.
If left untreated, about 30 percent of patients who have PE will die. Most of those who die do so within the first few hours of the event.
The good news is that a prompt diagnosis and proper treatment can save lives and help prevent the complications of PE.
Major Causes
Pulmonary embolism (PE) usually begins as a blood clot in a deep vein of the leg. This condition is called deep vein thrombosis. The clot can break free, travel through the bloodstream to the lungs, and block an artery.
Blood clots can form in the deep veins of the legs if blood flow is restricted and slows down. This can happen if you don’t move around for long periods, such as:
- After some types of surgery
- During a long trip in a car or airplane
- If you must stay in bed for an extended time
Blood clots are more likely to develop in veins damaged from surgery or injured in other ways.
Other Causes
Rarely, an air bubble, part of a tumor, or other tissue travels to the lungs and causes PE. Also, if a large bone in the body (such as the thigh bone) breaks, fat from the bone marrow can travel through the blood. If the fat reaches the lungs, it can cause PE
Pulmonary embolism (PE) occurs equally in men and women. The risk increases with age. For every 10 years after age 60, the risk of having PE doubles.
Certain inherited conditions, such as factor V Leiden, increase the risk of blood clotting and PE.
Major Risk Factors
Your risk for PE is high if you have deep vein thrombosis (DVT) or a history of DVT. In DVT, blood clots form in the deep veins of the body—most often in the legs. These clots can break free, travel through the bloodstream to the lungs, and block an artery.
Your risk for PE also is high if you’ve had the condition before.
Other Risk Factors
Other factors also can increase the risk for PE, such as:
- Being bedridden or unable to move around much
- Having surgery or breaking a bone (the risk goes up in the weeks following the surgery or injury)
- Having certain diseases or conditions, such as a stroke, paralysis (an inability to move), chronic heart disease, or high blood pressure
- Smoking
People who have recently been treated for cancer or who have a central venous catheter are more likely to develop DVT, which increases their risk for PE. A central venous catheter is a tube placed in a vein to allow easy access to the bloodstream for medical treatment.
Other risk factors for DVT include sitting for long periods (such as during long car or airplane rides), pregnancy and the 6-week period after pregnancy, and being overweight or obese. Women who take hormone therapy pills or birth control pills also are at increased risk for DVT.
The risk of developing blood clots increases as your number of risk factors increases.
Major Signs and Symptoms
Signs and symptoms of pulmonary embolism (PE) include unexplained shortness of breath, problems breathing, chest pain, coughing, or coughing up blood. An arrhythmia (irregular heartbeat) also may suggest that you have PE.
Sometimes the only signs and symptoms are related to deep vein thrombosis (DVT). These include swelling of the leg or along a vein in the leg, pain or tenderness in the leg, a feeling of increased warmth in the area of the leg that’s swollen or tender, and red or discolored skin on the affected leg.
See your doctor right away if you have any signs or symptoms of PE or DVT. It’s also possible to have PE and not have any signs or symptoms.
Other Signs and Symptoms
Some people who have PE have feelings of anxiety or dread, light-headedness or fainting, rapid breathing, sweating, or an increased heart rate.
Preventing pulmonary embolism (PE) begins with preventing deep vein thrombosis (DVT). Knowing whether you’re at risk for DVT and taking steps to lower your risk are important.
- Exercise your lower leg muscles if you’re sitting for a long time while traveling.
- Get out of bed and move around as soon as you’re able after having surgery or being ill. The sooner you move around, the better your chance is of avoiding a blood clot.
- Take medicines to prevent clots after some types of surgery (as your doctor prescribes).
- Follow up with your doctor.
If you’ve already had DVT or PE, you can take more steps to prevent new blood clots from forming. Visit your doctor for regular checkups. Also, use compression stockings to prevent chronic (ongoing) swelling in your legs from DVT (as your doctor advises).
Contact your doctor right away if you have any signs or symptoms of DVT or PE.
Pulmonary embolism (PE) is diagnosed based on your medical history, a physical exam, and test results.
Doctors who treat patients in the emergency room often are the ones to diagnose PE with the help of a radiologist. A radiologist is a doctor who deals with x rays and other similar tests.
Medical History and Physical Exam
To diagnose PE, the doctor will ask about your medical history. He or she will want to:
- Find out your deep vein thrombosis(DVT) and PE risk factors
- See how likely it is that you could have PE
- Rule out other possible causes for your symptoms
Your doctor also will do a physical exam. During the exam, he or she will check your legs for signs of DVT. He or she also will check your blood pressure and your heart and lungs.
Diagnostic Tests
Many tests can help diagnose PE. Which tests you have will depend on how you feel when you get to the hospital, your risk factors, available testing options, and other conditions you could possibly have. You may have one or more of the following tests.
Ultrasound
Doctors can use ultrasound to look for blood clots in your legs. Ultrasound uses sound waves to check blood flow in your veins.
For this test, gel is put on the skin of your legs. A hand-held device called a transducer is moved back and forth over the affected areas. The transducer gives off ultrasound waves and detects their echoes as they bounce off the vein walls and blood cells.
A computer turns the echoes into a picture on a computer screen, allowing the doctor to see blood flow in your legs. If the doctor finds blood clots in the deep veins of your legs, he or she will recommend treatment.
DVT and PE both are treated with the same medicines.
Computed Tomography Scans
Doctors can use computed tomography (to-MOG-rah-fee) scans, or CT scans, to look for blood clots in the lungs and legs.
For this test, dye is injected into a vein in your arm. The dye makes the blood vessels in your lungs and legs show up on x-ray images. You’ll lie on a table, and an x-ray tube will rotate around you. The tube will take pictures from many angles.
This test allows doctors to detect most cases of PE. The test only takes a few minutes. Results are available shortly after the scan is done.
Lung Ventilation/Perfusion Scan
A lung ventilation/perfusion scan, or VQ scan, uses a radioactive substance to show how well oxygen and blood are flowing to all areas of your lungs. This test can help detect PE.
Pulmonary Angiography
Pulmonary angiography (an-jee-OG-rah-fee) is another test used to diagnose PE. This test isn’t available at all hospitals, and a trained specialist must do the test.
For this test, a flexible tube called a catheter is threaded through the groin (upper thigh) or arm to the blood vessels in the lungs. Dye is injected into the blood vessels through the catheter.
X-ray pictures are taken to show blood flowing through the blood vessels in the lungs. If a blood clot is found, your doctor may use the catheter to remove it or deliver medicine to dissolve it.
Blood Tests
Certain blood tests may help your doctor find out whether you’re likely to have PE.
A D-dimer test measures a substance in the blood that’s released when a blood clot breaks down. High levels of the substance may mean a clot is present. If your test is normal and you have few risk factors, PE isn’t likely.
Other blood tests check for inherited disorders that cause blood clots. Blood tests also can measure the amount of oxygen and carbon dioxide in your blood. A clot in a blood vessel in your lungs may lower the level of oxygen in your blood.
Other Tests
To rule out other possible causes of your symptoms, your doctor may use one or more of the following tests.
- Echocardiography(echo). This test uses sound waves to create a moving picture of your heart. Doctors use echo to check heart function and detect blood clots inside the heart.
- EKG(electrocardiogram). An EKG is a simple, painless test that detects and records the heart’s electrical activity.
- Chest x ray. This test creates pictures of your lungs, heart, large arteries, ribs, and diaphragm (the muscle below your lungs).
- Chest MRI(magnetic resonance imaging). This test uses radio waves and magnetic fields to create pictures of organs and structures inside the body. MRI often can provide more information than an x ray.
Pulmonary embolism (PE) is treated with medicines, procedures, and other therapies. The main goals of treating PE are to stop the blood clot from getting bigger and keep new clots from forming.
Treatment may include medicines to thin the blood and slow its ability to clot. If your symptoms are life threatening, your doctor may give you medicine to quickly dissolve the clot. Rarely, your doctor may use surgery or another procedure to remove the clot.
Medicines
Anticoagulants (AN-te-ko-AG-u-lants), or blood thinners, decrease your blood’s ability to clot. They’re used to stop blood clots from getting larger and prevent clots from forming. Blood thinners don’t break up blood clots that have already formed. (The body dissolves most clots with time.)
You can take blood thinners as either a pill, an injection, or through a needle or tube inserted into a vein (called intravenous, or IV, injection). Warfarin is given as a pill. (Coumadin® is a common brand name for warfarin.) Heparin is given as an injection or through an IV tube.
Your doctor may treat you with both heparin and warfarin at the same time. Heparin acts quickly. Warfarin takes 2 to 3 days before it starts to work. Once warfarin starts to work, heparin usually is stopped.
Pregnant women usually are treated with heparin only, because warfarin is dangerous for the pregnancy.
If you have deep vein thrombosis, treatment with blood thinners usually lasts for 3 to 6 months. If you’ve had blood clots before, you may need a longer period of treatment. If you’re being treated for another illness, such as cancer, you may need to take blood thinners as long as PE risk factors are present.
The most common side effect of blood thinners is bleeding. This can happen if the medicine thins your blood too much. This side effect can be life threatening.
Sometimes the bleeding is internal, which is why people treated with blood thinners usually have routine blood tests. These tests, called PT and PTT tests, measure the blood’s ability to clot. These tests also help your doctor make sure you’re taking the right amount of medicine. Call your doctor right away if you’re bruising or bleeding easily.
Thrombin inhibitors are a newer type of blood-thinning medicine. They’re used to treat some types of blood clots in people who can’t take heparin.
Emergency Treatment
When PE is life threatening, a doctor may use treatments that remove or break up the blood clot. These treatments are given in an emergency room or hospital.
Thrombolytics (THROM-bo-LIT-iks) are medicines that can quickly dissolve a blood clot. They’re used to treat large clots that cause severe symptoms. Because thrombolytics can cause sudden bleeding, they’re used only in life-threatening situations.
Sometimes a doctor may use a catheter (a flexible tube) to reach the blood clot. The catheter is inserted into a vein in the groin (upper thigh) or arm and threaded to the clot in the lung. The doctor may use the catheter to remove the clot or deliver medicine to dissolve it.
Rarely, surgery may be needed to remove the blood clot.
Other Types of Treatment
If you can’t take medicines to thin your blood, or if the medicines don’t work, your doctor may suggest a vena cava filter. This device keeps blood clots from traveling to your lungs.
The filter is inserted inside a large vein called the inferior vena cava. (This vein carries blood from the body back to the heart). The filter catches clots before they travel to the lungs. This type of treatment can prevent PE, but it won’t stop other blood clots from forming.
Graduated compression stockings can reduce the chronic (ongoing) swelling that a blood clot in the leg may cause.
Graduated compression stockings are worn on the legs from the arch of the foot to just above or below the knee. These stockings are tight at the ankle and become looser as they go up the leg. This causes gentle compression (pressure) up the leg. The pressure keeps blood from pooling and clotting.
Pulmonary embolism (PE) usually is treated in a hospital. After leaving the hospital, you may need to take medicine at home for 6 months or longer. It’s important to:
- Take all medicines as prescribed, and have blood tests done as your doctor advises.
- Talk with your doctor before taking blood-thinning medicines with any other medicines, including over-the-counter products. Over-the-counter aspirin, for example, can thin your blood. Taking two medicines that thin your blood may increase your risk of bleeding.
- Ask your doctor about your diet. Foods that contain vitamin K can affect how well warfarin (Coumadin®) works. Vitamin K is found in green leafy vegetables and some oils, such as canola and soybean oils. It’s best to eat a well-balanced, healthy diet.
- Discuss with your doctor what amount of alcohol is safe for you to drink if you’re taking medicine.
Medicines used to treat PE can thin your blood too much. This can cause bleeding in the digestive system or the brain. If you have signs or symptoms of bleeding in the digestive system or the brain, get treatment at once.
Signs and symptoms of bleeding in the digestive system include:
- Bright red vomit or vomit that looks like coffee grounds
- Bright red blood in your stool or black, tarry stools
- Pain in your abdomen
Signs and symptoms of bleeding in the brain include:
- Severe pain in your head
- Sudden changes in your vision
- Sudden loss of movement in your legs or arms
- Memory loss or confusion
Excessive bleeding from a fall or injury also may mean that your PE medicines have thinned your blood too much. Excessive bleeding is bleeding that won’t stop after you apply pressure to a wound for 10 minutes. If you have excessive bleeding from a fall or injury, get treatment at once.
Once you’ve had PE (with or without deep vein thrombosis (DVT)), you’re at higher risk of having the condition again. During treatment and after, continue to take steps to prevent DVT.
Check your legs for any signs or symptoms of DVT, such as swollen areas, pain or tenderness, increased warmth in swollen or painful areas, or red or discolored skin.
If you think that you have DVT or are having symptoms of PE, contact your doctor right away.
The National Heart, Lung, and Blood Institute (NHLBI) leads or sponsors many studies aimed at preventing, diagnosing, and treating heart, lung, blood, and sleep disorders.
Learn more about participating in a clinical trial.
View all trials from ClinicalTrials.govexternal link.
Visit Children and Clinical Studiesexternal link to hear experts, parents, and children talk about their experiences with clinical research.
The information contained in materials published by the National Heart, Lung, and Blood Institute (NHLBI) is in the public domain. No further permission is required to reproduce or reprint the information in whole or in part. However, organizations that reproduce NHLBI publications should cite the National Heart, Lung, and Blood Institute as a part of the National Institutes of Health and the U.S. Department of Health and Human Services as the source. This applies to printed publications as well as documents from the NHLBI Web site. Organizations may add their own logo or name. We further ask that no changes be made in the content of the material, and that the material as well as any NHLBI Internet links should not be used in any direct or indirect product endorsement or advertising.
All NINDS-prepared information is in the public domain and may be freely copied. Credit to the NINDS or the NIH is appreciated Where to find on the internet: http://www.nhlbi.nih.gov/health/dci/Diseases/pe/pe_what.html
Our Mission

Founded in 2005, the APS Foundation of America, Inc. is dedicated to fostering and facilitating joint efforts in the areas of education, public awareness, research, and patient services for Antiphospholipid Syndrome (APS) in an effective and ethical manner.
Information Sheets
DISCLAIMER: The APS Foundation of America, Inc. website is not intended to replace standard doctor-patient visits, physical examination, and medical testing. Information given to members is only an opinion. All information should be confirmed with your doctor. Always seek a trained physician's advice before seeking any new treatment regarding your medical diagnosis or condition. Any information received from the APS Foundation of America, Inc. website is not intended to diagnose, treat, or cure. This site is for informational purposes only. Please note that we will list all donors' or purchasers' names on the donor page of our foundation site. If you do not want your name listed, please get in touch with us to opt-out. If you think you may have a medical emergency, call your doctor or 911 immediately.
