Heart Attack
A heart attack happens when the flow of oxygen-rich blood to a section of heart muscle suddenly becomes blocked and the heart can’t get oxygen. If blood flow isn’t restored quickly, the section of heart muscle begins to die.
Heart attack treatment works best when it’s given right after symptoms occur. If you think you or someone else is having a heart attack, even if you’re not sure, call 911 right away.
Other names:
- Myocardial infarction (MI)
- Acute myocardial infarction (AMI)
- Acute coronary syndrome
- Coronary thrombosis
- Coronary occlusion
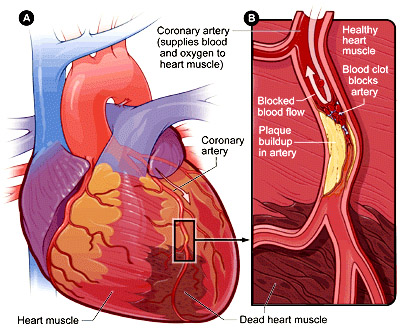
Figure A is an overview of a heart and coronary artery showing damage (dead heart muscle) caused by a heart attack. Figure B is a cross-section of the coronary artery with plaque buildup and a blood clot.
Source: National Heart, Lung, and Blood Institute; National Institutes of Health; U.S. Department of Health and Human Services.
Certain risk factors make it more likely that you’ll develop coronary heart disease (CHD) and have a heart attack. You can control many of these risk factors.
Risk Factors You Can Control
The major risk factors for a heart attack that you can control include:
- Smoking
- High blood pressure
- High blood cholesterol
- Overweight and obesity
- An unhealthy diet (for example, a diet high in saturated fat, trans fat, cholesterol, and sodium)
- Lack of routine physical activity
- High blood sugar due to insulin resistance or diabetes
Some of these risk factors—such as obesity, high blood pressure, and high blood sugar—tend to occur together. When they do, it’s called metabolic syndrome.
In general, a person who has metabolic syndrome is twice as likely to develop heart disease and five times as likely to develop diabetes as someone who doesn’t have metabolic syndrome.
For more information about the risk factors that are part of metabolic syndrome, go to the Health Topics Metabolic Syndrome article.
Risk Factors You Can’t Control
Risk factors that you can’t control include:
- Age. The risk of heart disease increases for men after age 45 and for women after age 55 (or after menopause).
- Family history of early heart disease. Your risk increases if your father or a brother was diagnosed with heart disease before 55 years of age, or if your mother or a sister was diagnosed with heart disease before 65 years of age.
- Preeclampsia (pre-e-KLAMP-se-ah). This condition can develop during pregnancy. The two main signs of preeclampsia are a rise in blood pressure and excess protein in the urine. Preeclampsia is linked to an increased lifetime risk of heart disease, including CHD, heart attack, heart failure, and high blood pressure.
Coronary Heart Disease
A heart attack happens if the flow of oxygen-rich blood to a section of heart muscle suddenly becomes blocked and the heart can’t get oxygen. Most heart attacks occur as a result of coronary heart disease (CHD).
CHD is a condition in which a waxy substance called plaque builds up inside of the coronary arteries. These arteries supply oxygen-rich blood to your heart.
When plaque builds up in the arteries, the condition is called atherosclerosis. The buildup of plaque occurs over many years.
Eventually, an area of plaque can rupture (break open) inside of an artery. This causes a blood clot to form on the plaque’s surface. If the clot becomes large enough, it can mostly or completely block blood flow through a coronary artery.
If the blockage isn’t treated quickly, the portion of heart muscle fed by the artery begins to die. Healthy heart tissue is replaced with scar tissue. This heart damage may not be obvious, or it may cause severe or long-lasting problems.
Coronary Artery Spasm
A less common cause of heart attack is a severe spasm (tightening) of a coronary artery. The spasm cuts off blood flow through the artery. Spasms can occur in coronary arteries that aren’t affected by atherosclerosis.
What causes a coronary artery to spasm isn’t always clear. A spasm may be related to:
- Taking certain drugs, such as cocaine
- Emotional stress or pain
- Exposure to extreme cold
Not all heart attacks begin with the sudden, crushing chest pain that often is shown on TV or in the movies. In one study, for example, one-third of the patients who had heart attacks had no chest pain. These patients were more likely to be older, female, or diabetic.
The symptoms of a heart attack can vary from person to person. Some people can have few symptoms and are surprised to learn they’ve had a heart attack. If you’ve already had a heart attack, your symptoms may not be the same for another one. It is important for you to know the most common symptoms of a heart attack and also remember these facts:
- Heart attacks can start slowly and cause only mild pain or discomfort. Symptoms can be mild or more intense and sudden. Symptoms also may come and go over several hours.
- People who have high blood sugar (diabetes) may have no symptoms or very mild ones.
- The most common symptom, in both men and women, is chest pain or discomfort.
- Women are somewhat more likely to have shortness of breath, nausea and vomiting, unusual tiredness (sometimes for days), and pain in the back, shoulders, and jaw.
Some people don’t have symptoms at all. Heart attacks that occur without any symptoms or with very mild symptoms are called silent heart attacks.
Most Common Symptoms
The most common warning symptoms of a heart attack for both men and women are:
- Chest pain or discomfort. Most heart attacks involve discomfort in the center or left side of the chest. The discomfort usually lasts for more than a few minutes or goes away and comes back. It can feel like pressure, squeezing, fullness, or pain. It also can feel like heartburn or indigestion. The feeling can be mild or severe.
- Upper body discomfort. You may feel pain or discomfort in one or both arms, the back, shoulders, neck, jaw, or upper part of the stomach (above the belly button).
- Shortness of breath. This may be your only symptom, or it may occur before or along with chest pain or discomfort. It can occur when you are resting or doing a little bit of physical activity.
The symptoms of angina (an-JI-nuh or AN-juh-nuh) can be similar to the symptoms of a heart attack. Angina is chest pain that occurs in people who have coronary heart disease, usually when they’re active. Angina pain usually lasts for only a few minutes and goes away with rest.
Chest pain or discomfort that doesn’t go away or changes from its usual pattern (for example, occurs more often or while you’re resting) can be a sign of a heart attack.
All chest pain should be checked by a doctor.
Other Common Signs and Symptoms
Pay attention to these other possible symptoms of a heart attack:
- Breaking out in a cold sweat
- Feeling unusually tired for no reason, sometimes for days (especially if you are a woman)
- Nausea (feeling sick to the stomach) and vomiting
- Light-headedness or sudden dizziness
- Any sudden, new symptoms or a change in the pattern of symptoms you already have (for example, if your symptoms become stronger or last longer than usual)
Not everyone having a heart attack has typical symptoms. If you’ve already had a heart attack, your symptoms may not be the same for another one. However, some people may have a pattern of symptoms that recur.
The more signs and symptoms you have, the more likely it is that you’re having a heart attack.
Quick Action Can Save Your Life: Call 911
The signs and symptoms of a heart attack can develop suddenly. However, they also can develop slowly—sometimes within hours, days, or weeks of a heart attack.
Any time you think you might be having heart attack symptoms or a heart attack, don’t ignore it or feel embarrassed to call for help. Call 911 for emergency medical care, even if you are not sure whether you’re having a heart attack. Here’s why:
- Acting fast can save your life.
- An ambulance is the best and safest way to get to the hospital. Emergency medical services (EMS) personnel can check how you are doing and start life-saving medicines and other treatments right away. People who arrive by ambulance often receive faster treatment at the hospital.
- The 911 operator or EMS technician can give you advice. You might be told to crush or chew an aspirin if you’re not allergic, unless there is a medical reason for you not to take one. Aspirin taken during a heart attack can limit the damage to your heart and save your life.
Every minute matters. Never delay calling 911 to take aspirin or do anything else you think might help.
Lowering your risk factors for coronary heart disease can help you prevent a heart attack. Even if you already have coronary heart disease, you still can take steps to lower your risk for a heart attack. These steps involve making heart-healthy lifestyle changes and getting ongoing medical care for related conditions that make heart attack more likely. Talk to your doctor about whether you may benefit from aspirin primary prevention, or using aspirin to help prevent your first heart attack.
Heart-Healthy Lifestyle Changes
A heart-healthy lifestyle can help prevent a heart attack and includes heart-healthy eating, being physically active, quitting smoking, managing stress, and managing your weight.
Ongoing Care
Treat Related Conditions
Treating conditions that make a heart attack more likely also can help lower your risk for a heart attack. These conditions may include:
- Diabetes (high blood sugar). If you have diabetes, try to control your blood sugar level through diet and physical activity (as your doctor recommends). If needed, take medicine as prescribed.
- High blood cholesterol. Your doctor may prescribe a statin medicine to lower your cholesterol if diet and exercise aren’t enough.
- High blood pressure. Your doctor may prescribe medicine to keep your blood pressure under control.
- Chronic kidney disease. Your doctor may prescribe medicines to control your high blood pressure or high blood sugar levels.
- Peripheral artery disease. Your doctor may recommend surgery or procedures to unblock the affected arteries.
Have an Emergency Action Plan
Make sure that you have an emergency action plan in case you or someone in your family has a heart attack. This is very important if you’re at high risk for, or have already had, a heart attack.
Write down a list of medicines you are taking, medicines you are allergic to, your health care provider’s phone numbers (both during and after office hours), and contact information for a friend or relative. Keep the list in a handy place (for example, fill out this wallet card) to share in a medical emergency.
Talk with your doctor about the signs and symptoms of a heart attack, when you should call 9–1–1, and steps you can take while waiting for medical help to arrive.
The National Heart, Lung, and Blood Institute (NHLBI) leads or sponsors many studies aimed at preventing, diagnosing, and treating heart, lung, blood, and sleep disorders.
Learn more about participating in a clinical trial.
View all trials from ClinicalTrials.govexternal link .
Visit Children and Clinical Studiesexternal link to hear experts, parents, and children talk about their experiences with clinical research.
NHLBI Resources
- Aim for a Healthy Weight
- Don’t Take a Chance With a Heart Attack: Know the Facts and Act Fast
- Heart Attack: Know the Symptoms. Take Action. Wallet Card
- In Brief: Your Guide to Lowering Your Blood Pressure With DASH
- Learn What a Heart Attack Feels Like—It Could Save Your Life
- The Heart Truth®for Women Campaign
Non-NHLBI Resources
- Angina (MedlinePlus)
- Cigarette and Tobacco Factsexternal link (National Institute on Drug Abuse)
- Coronary Artery Disease (MedlinePlus)
- Heart Attack (MedlinePlus)
Prepared by:
National Heart, Lung, and Blood Institute; National Institutes of Health; U.S. Department of Health and Human Services.
NHLBI health-related material is provided for information purposes only and does not necessarily represent endorsement by or an official position of the National Heart, Lung, and Blood Institute; National Institutes of Health; U.S. Department of Health and Human Services; or any other Federal agency. Advice on the treatment or care of an individual patient should be obtained through consultation with a physician who has examined that patient or is familiar with that patient’s medical history.
All NHLBI-prepared information is in the public domain and may be freely copied. Credit to the NHLBI or the NIH is appreciated Where to find on the internet: https://www.nhlbi.nih.gov/health-topics/heart-attack
Our Mission

Founded in 2005, the APS Foundation of America, Inc. is dedicated to fostering and facilitating joint efforts in the areas of education, public awareness, research, and patient services for Antiphospholipid Syndrome (APS) in an effective and ethical manner.
Information Sheets
DISCLAIMER: APS Foundation of America, Inc. website is not intended to replace standard doctor-patient visits, physical examination, and medical testing. Information given to members is only an opinion. All information should be confirmed with your personal doctor. Always seek the advice of a trained physician in person before seeking any new treatment regarding your medical diagnosis or condition. Any information received from APS Foundation of America, Inc. website is not intended to diagnose, treat, or cure. This site is for informational purposes only. Please note that we will be listing all donor or purchaser's names on the Donor page of our foundation site. If you do not want your name listed, please contact us to opt out. If you think you may have a medical emergency, call your doctor or 911 immediately.
